The woman’s mysterious symptoms started in her stomach.
Weeks of abdominal pain and diarrhea led to night sweats and a dry cough. Then, doctors found lesions on her lungs, liver and spleen. An infection, perhaps. But tests for bacteria, fungi, a human parasite and even autoimmune disease all came up negative.
Three weeks later, the woman was in the hospital with a fever and cough. CT scans revealed a clue that was telling, in retrospect: Some of her lung lesions appeared to be migrating. A second clue came months later, when the woman became forgetful and depressed. “She had a very astute GP who thought, ‘Something’s not right here, I better do an MRI of the brain,’” says Sanjaya Senanayake, an infectious disease physician at the Australian National University and the Canberra Hospital.
That brain scan turned up a ghostly glow in her frontal lobe. It could have been cancer, an abscess or another affliction, Senanayake says. “No one thought it was going to be a worm.”
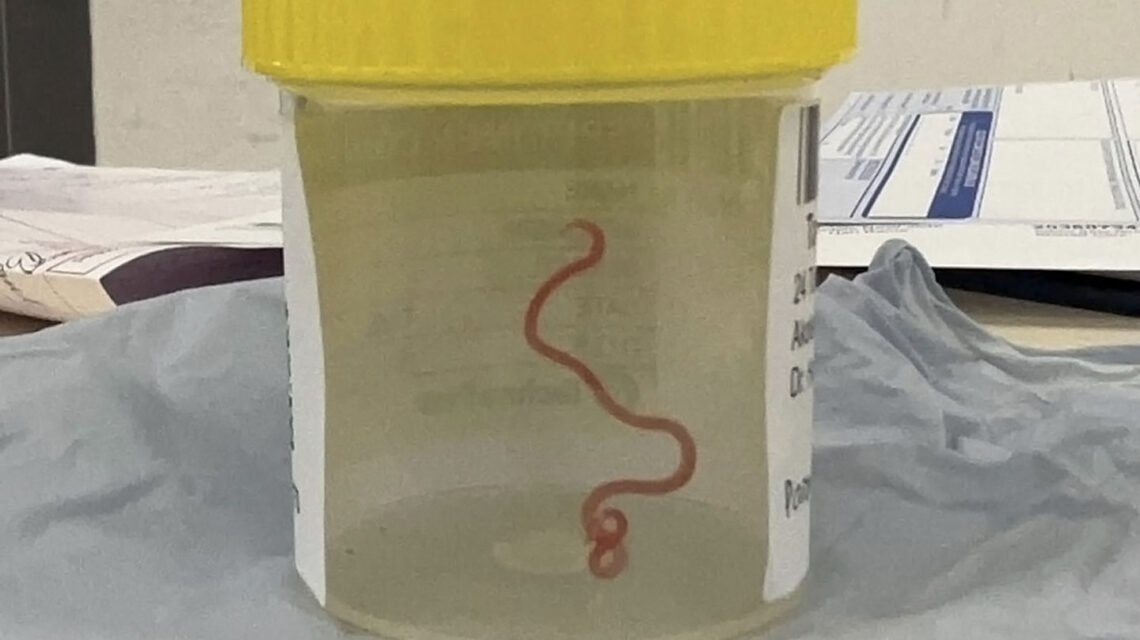
During a biopsy of the woman’s brain, her neurosurgeon spotted a suspicious stringlike structure and plucked it out with forceps. It was pinkish-red, about half the length of a pencil — and still alive.
“It was definitely one of those ‘wow’ moments,” Senanayake says. “A worm in the brain!” But the doctors also felt relieved. It meant they had a diagnosis, he says. The team finally would know how to treat its patient.
The worm, Ophidascaris robertsi, was a nematode whose main host is a snake, Senanayake and his colleagues report in the September Emerging Infectious Diseases. The woman, who lives in New South Wales, Australia, is the first documented case of an infection in humans.
“The live wriggling worm was … what got everyone so interested,” Senanayake says, “but there’s a more important side to it.” O. robertsi is a parasite that jumped from wild animals to a human. As human and animal populations overlap, he says, “we’re…
Read the full article here